
Mental health transformation: 47% respond to psychedelic therapy
TL;DR:
- Psychedelic-assisted therapies can induce rapid, lasting mental health transformations surpassing traditional treatments.
- The process involves preparation, guided sessions, and integration to ensure durable change.
- Proper screening and professional guidance are essential to manage risks and maximize benefits.
Most people assume healing is slow. You try a medication, wait weeks, adjust the dose, wait again. Therapy helps, but progress can feel like watching paint dry. What if that assumption is wrong? Psychedelic-assisted therapies have demonstrated rapid, sometimes dramatic results in cases where conventional treatments have repeatedly fallen short. We’re not talking about fringe science. We’re talking about peer-reviewed, clinically tested approaches that are reshaping what mental health transformation actually looks like. This article will walk you through what transformation really means, how these therapies work, and what the evidence honestly shows.
Table of Contents
- Defining mental health transformation
- How psychedelic-assisted therapy enables profound change
- Clinical evidence: Outcomes, durability, and comparison
- Risks, nuances, and evolving debates
- Why true transformation demands rigorous guidance and an open mind
- Take the next step toward transformation
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Transformation is possible | Psychedelic-assisted therapies can rapidly spark deep emotional and psychological change where traditional approaches often stall. |
| Neurobiology matters | These therapies work through unique brain mechanisms, combining chemical and experiential effects for sustainable impact. |
| Safety requires guidance | Careful preparation, expert support, and proper integration are crucial for lasting benefits and risk reduction. |
| Evidence-driven optimism | Clinical results with psilocybin and DMT show high response rates, especially in treatment-resistant cases. |
| Transformation is ongoing | Real change extends beyond the session—ongoing integration and personal commitment are essential. |
Defining mental health transformation
The word “transformation” gets used loosely. In mental health, it can mean anything from sleeping better to feeling like a fundamentally different person. So let’s be precise about what we mean.
At its broadest, mental health transformation refers to meaningful, lasting shifts in how you think, feel, and engage with the world. It’s not just symptom reduction. It’s a change in the underlying patterns that drive suffering. Think of it as the difference between turning down the volume on pain versus rewiring the speaker itself.
Organizations like the World Health Organization and SAMHSA frame transformation at a systemic level, emphasizing community integration, policy reform, and the inclusion of lived experience in shaping care. That perspective matters enormously for public health. But it doesn’t always speak to what you need when you’re sitting with depression that won’t lift.
Psychedelic-assisted therapy approaches transformation differently. Here, the focus is on profound shifts in brain connectivity and individual worldview. The goal is to create a window, often brief but powerful, where the mind becomes more flexible and open to change. That flexibility is where healing can take root.
Here’s how these two approaches differ in practice:
- Systemic transformation: Policy change, community support, reducing stigma, reforming care access
- Individual transformation: Rewiring neural patterns, shifting emotional responses, gaining new perspectives on trauma
- What they share: Both recognize that lasting change requires more than a prescription and a waiting room
Understanding this distinction matters because it helps you ask the right question: What kind of transformation are you actually seeking? If you’re looking for a fundamental shift in how you experience yourself and the world, the cultural context of transformation also plays a role. Healing doesn’t happen in a vacuum. Your background, values, and relationships all shape what transformation means for you.
“Mental health transformation in psychedelic-assisted therapy isn’t about escaping yourself. It’s about finally being able to meet yourself clearly, perhaps for the first time.”
That clarity is what makes this field so compelling, and so worth understanding deeply.
How psychedelic-assisted therapy enables profound change
Knowing that transformation is possible is one thing. Understanding how it happens is another. Psychedelic-assisted therapy isn’t just about the experience during a session. It’s a carefully structured process built around three essential phases.
The three-phase protocol works like this:
- Preparation: You and your care team build trust, clarify intentions, and address any psychological or medical concerns before the session. This phase sets the container for everything that follows.
- Administration: The psychedelic session itself, conducted in a safe, supported environment with trained guides or clinicians present. This is where the neurobiological shifts occur.
- Integration: The work that happens after. Processing what emerged, translating insights into lasting behavioral change, and consolidating new neural pathways.
On a neurobiological level, psychedelics like psilocybin act primarily through 5-HT2A receptor agonism and default mode network disruption. The default mode network, or DMN, is the brain’s “autopilot” system. It’s heavily involved in rumination, self-referential thinking, and the rigid mental loops that sustain depression and anxiety. When psychedelics temporarily quiet this network, the brain can form new connections. This is neuroplasticity in action.

Beyond the biology, there’s the phenomenological experience. Many people describe a loosening of the ego, a sense that the boundaries between self and world soften. This isn’t disorientation for its own sake. It creates space for fresh perspectives on old wounds, old stories, and old patterns of thinking.
This is where mindful preparation becomes genuinely important. The more grounded and intentional you are going in, the more meaningful and navigable the experience tends to be.
Pro Tip: Don’t underestimate the integration phase. Many people focus all their energy on the session itself, but the weeks following are where the real transformation gets anchored. Journaling, therapy, and community support during this period make a measurable difference.
Compared to standard talk therapy or daily medication, this protocol is strikingly different. Conventional approaches often require months or years of consistent effort to produce meaningful change. Psychedelic therapy compresses that window, sometimes dramatically.
Clinical evidence: Outcomes, durability, and comparison
Let’s talk numbers, because the data here is genuinely striking.
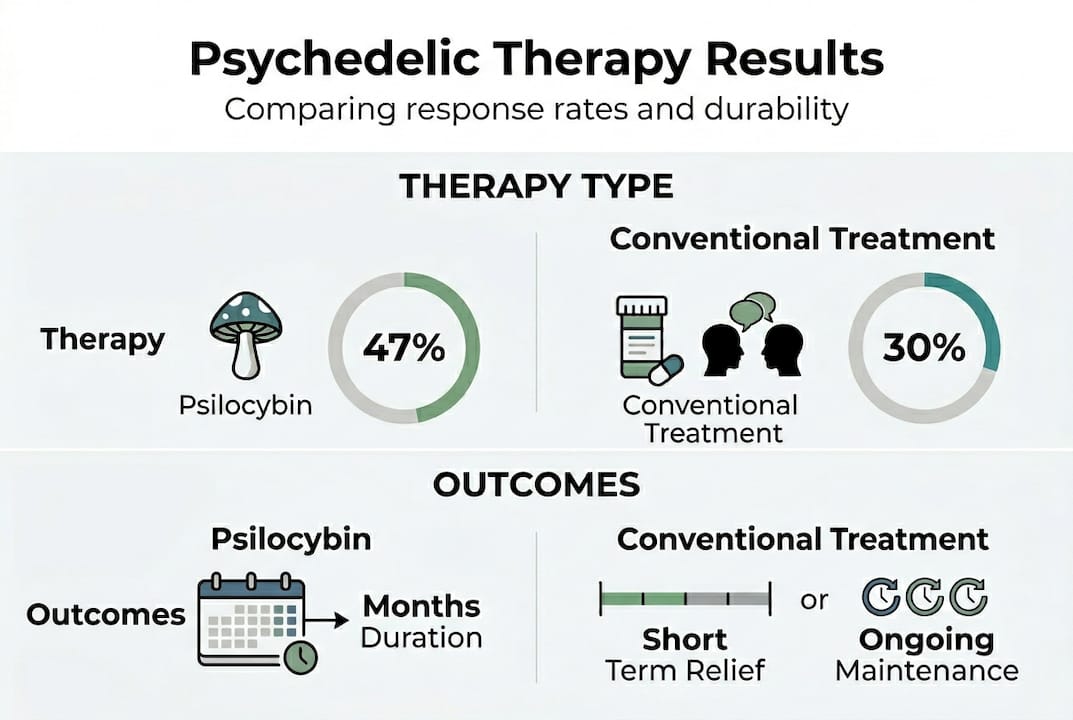
Psilocybin single-dose trials show response rates between 47% and 60% in treatment-resistant depression. Pilot data involving DMT and veterans populations are also showing promising early results. These aren’t marginal improvements. For people who have tried multiple medications without relief, these numbers represent something profound.
| Therapy type | Response rate | Durability | Best suited for |
|---|---|---|---|
| Psilocybin-assisted | 47-60% | Months to over a year | TRD, existential distress |
| DMT-assisted | Early data positive | Under study | PTSD, depression |
| Ketamine/Spravato | Rapid onset | Shorter duration | Acute suicidality, TRD |
| Standard antidepressants | 40-60% | Ongoing use required | Broad depression/anxiety |
| Talk therapy alone | Variable | Durable with practice | Mild to moderate cases |
What stands out in this comparison is durability. Empirical benchmarks favor psilocybin and DMT over ketamine for long-term remission in treatment-resistant depression, or TRD. Ketamine works fast, which matters enormously in crisis situations, but its effects often require repeat dosing to sustain. Psilocybin, in contrast, can produce lasting relief from just one or two sessions.
Factors that influence outcomes include:
- The specific molecule used (psilocybin, MDMA, DMT, ketamine each have different profiles)
- Diagnosis and severity (treatment-resistant cases often respond differently than first-line)
- Level of therapeutic support (guided vs. minimal support shows significant outcome differences)
- Individual biology and psychological readiness
What do these numbers mean in plain terms? If you’ve tried two or more antidepressants without adequate relief, you may be in the population where evidence for psychedelic therapies shows the most compelling advantage. That’s not a guarantee. But it is a reason to look seriously at these options.
Risks, nuances, and evolving debates
Honesty matters here. These therapies are powerful, and power cuts both ways.
The most common side effects include temporary dysphoria, anxiety during the session, and the re-engagement of difficult memories or trauma. For most people in well-designed programs, these are manageable and even therapeutically useful. But for some, they represent real risk.
PTSD and trauma patients may require significantly more support before, during, and after sessions. Risks in this population include deeper trauma re-engagement, emotional destabilization, and in rare cases, suicidal ideation. Careful screening is not optional. It’s essential.
Who should approach with extra caution or avoid these therapies entirely:
- People with personal or family history of schizophrenia or psychosis
- Those with severe, unprocessed trauma without adequate therapeutic support in place
- Individuals on medications with significant serotonin interactions
- Anyone in an acute mental health crisis without appropriate clinical oversight
Pro Tip: A reputable program will always conduct thorough intake screening. If a provider skips this step or minimizes it, that’s a serious red flag. Proper screening protects you.
The debates in this field are real and worth knowing about. Contrasting viewpoints exist on how much structured psychotherapy is actually required alongside the psychedelic experience. The FDA’s rejection of MDMA-assisted therapy for PTSD in 2024 was partly driven by concerns about the therapy component’s standardization and potential for bias. This doesn’t mean the approach is invalid. It means the field is still maturing.
Newer non-hallucinogenic analogs are also being studied, compounds that may offer some of the neuroplasticity benefits without the intense perceptual experience. These are promising but still early-stage. For now, holistic approaches to integration remain the gold standard for supporting safe, lasting outcomes.
Why true transformation demands rigorous guidance and an open mind
Here’s what I’ve come to believe, and what the evidence increasingly supports: the session itself is not the transformation. It’s a doorway.
Most people seeking psychedelic therapy focus intensely on the dosing experience. They want the breakthrough moment, the insight, the shift. And those moments are real. But the success of guided integration is what determines whether that doorway leads somewhere lasting or closes behind you.
Preparation and aftercare are not add-ons. They are the architecture of the transformation. Without them, even the most profound session can fade into a memory rather than a new way of living. I’ve seen this pattern clearly, and the research reflects it.
We also need to be honest about what we don’t yet know. Durability varies. Ethics matter. Standardization across programs is still inconsistent. Choosing a program that prioritizes transparency, ongoing research, and rigorous clinical standards isn’t just a preference. It’s a form of self-protection.
Transformation is a process, not a single event. The most meaningful changes tend to unfold over weeks and months, supported by skilled clinicians and a genuine commitment to showing up for yourself. If you’re exploring carefully designed transformation programs, look for ones that treat integration as seriously as the session itself.
Take the next step toward transformation
If you’ve been carrying the weight of treatment-resistant depression, trauma, or emotional pain that hasn’t responded to conventional approaches, you deserve more than another incremental adjustment.

At Mystic Health, we’ve built our approach around exactly what the evidence demands: expert-guided preparation, carefully supervised sessions, and deep integration support. Our explore available programs page walks you through every modality we offer, from ketamine-assisted therapy to Spravato. You can also explore our mindfulness course for integration to build the inner foundation that makes transformation stick. And if you want to understand the science behind what we do, our review the clinical evidence page lays it all out clearly. You don’t have to navigate this alone.
Frequently asked questions
What does ‘mental health transformation’ mean in psychedelic therapy?
It refers to profound emotional and psychological change sparked by guided psychedelic sessions, often leading to lasting symptom relief and shifts in how you perceive yourself and the world.
How fast do results appear with psychedelic therapy?
Improvements can emerge after one or two sessions, with benefits lasting months in many cases, though individual results vary based on diagnosis, support level, and the specific therapy used.
Is psychedelic-assisted therapy safe for everyone?
No. People with schizophrenia risk or severe trauma require careful screening, and some individuals may need alternative or more heavily supported approaches before considering psychedelic therapy.
What if I don’t live near a psychedelic therapy clinic?
Preparatory counseling, integration support, and mindfulness practices may be available remotely, but psychedelic dosing always requires in-person medical oversight and cannot be safely conducted outside a clinical setting.
How does psychedelic therapy compare to regular medication?
Research suggests that single or few psychedelic doses can provide faster and sometimes more durable relief, with psilocybin outperforming ketamine for long-term remission in treatment-resistant depression compared to standard medicines.
Recommended

Mystic Health Blog

FAQs
1. Am I eligible for ketamine therapy?
2. Does insurance cover the cost of ketamine therapy?
3. How many ketamine treatments will I need?
We recommend two initial treatments to determine suitability and adjust dosage. After these sessions, additional treatments are available based on your progress and specific requirements.








